Wound Care Doctor: Identifying Your Wound and Why It Matters
If you or a loved one is struggling with a stubborn or unfamiliar wound, knowing how to identify the type and understand its unique needs can make all the difference in recovery. At Wells Surgical Services LLC, our expert wound care doctor serving St. Augustine, FL, helps patients navigate wound healing with precision and care. This article will guide you through the most common chronic wounds, their causes, and key symptoms to watch for, and why tailored treatment is vital, so you can make informed decisions and recognize when urgent medical attention is necessary.
Understanding Common Chronic Wound Types
Chronic wounds are injuries that fail to progress through the normal healing stages within an expected timeframe, typically persisting beyond four to six weeks. Recognizing the type of wound is the first step in ensuring proper management, which is why a wound care doctor plays a pivotal role in your healing journey.
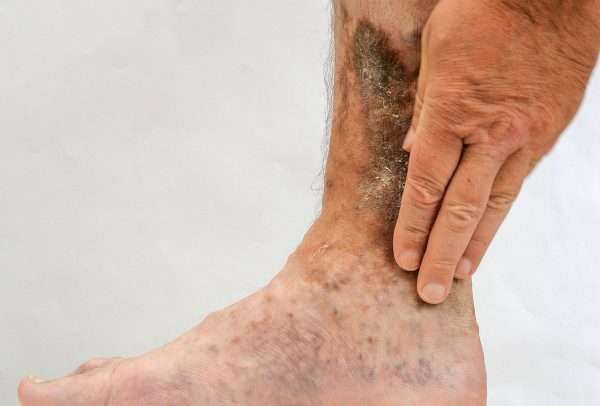
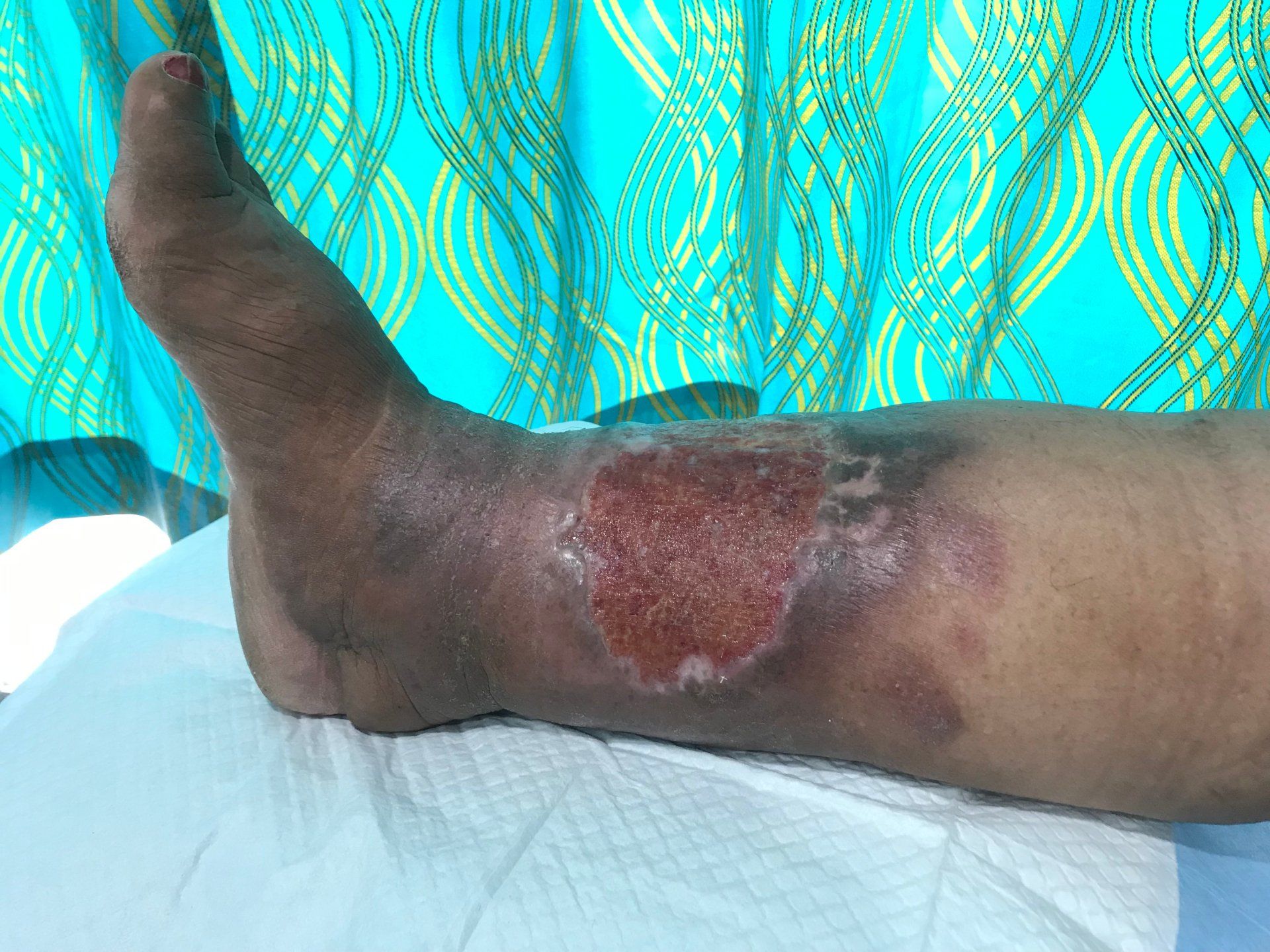
1. Venous (Stasis) Ulcers
Venous ulcers commonly develop in the lower legs due to poor blood flow caused by venous insufficiency. These wounds often appear irregularly shaped with a shallow base, surrounded by discolored or thickened skin. Symptoms typically include aching, swelling, and heaviness in the affected limb. Risk factors include varicose veins, obesity, and a history of deep vein thrombosis.
2. Diabetic Foot Ulcers
Diabetic ulcers are a major complication for individuals with diabetes, primarily forming on pressure points of the feet due to nerve damage (neuropathy) and poor circulation. These wounds can look deep, may be surrounded by calloused skin, and often show signs of infection such as redness, warmth, or discharge. Because patients may have reduced sensation, wounds can go unnoticed and worsen quickly.
3. Pressure Ulcers (Bedsores)
Pressure ulcers develop from prolonged pressure on the skin, especially in immobile individuals. They commonly affect bony prominences like the heels, hips, and tailbone. Early signs include redness or discoloration that doesn’t fade with pressure, progressing to open sores if untreated. Patients with limited mobility, such as those in nursing homes or recovering from surgery, are at higher risk.
4. Arterial (Ischemic) Ulcers
These ulcers result from poor arterial blood flow, usually appearing on the feet and toes. They tend to have a punched-out, round appearance with a pale or necrotic base. Patients may experience severe pain, especially when elevating the leg or resting, and symptoms can worsen with activity. Smoking, diabetes, and peripheral artery disease increase the risk.
Why Knowing Your Wound Type Matters
Each chronic wound type has a unique cause and healing environment, making tailored treatment essential for effective recovery. A wound care doctor understands these differences and uses precise diagnostic methods, such as physical examination, medical history review, and sometimes specialized imaging, to classify wounds accurately.
Treatments vary widely depending on the wound type.
For example:
- Venous ulcers often respond well to compression therapy to improve blood flow.
- Diabetic ulcers require offloading pressure and rigorous infection control.
- Pressure ulcers necessitate repositioning, skin protection, and nutritional support.
- Arterial ulcers may need vascular evaluation and interventions to restore blood flow.
Using appropriate therapies based on wound classification promotes faster healing, reduces complications, and enhances quality of life.
Risk Factors That Influence Wound Development
Several factors increase the likelihood of chronic or non-healing wounds, including:
- Poor circulation: from venous insufficiency or arterial disease.
- Diabetes: impairing nerve function and immune response.
- Immobility: leading to pressure injuries.
- Obesity: contributing to circulatory challenges.
- Age: older adults heal more slowly.
- Infections: produce inflammation and tissue damage.
- Smoking: reduces oxygen delivery to tissues.
Understanding and addressing these factors with your wound care doctor helps optimize healing outcomes.
Recognizing Red Flags That Require Urgent Evaluation
While many wounds can be safely managed with appropriate care, certain signs indicate the need for immediate professional evaluation:
- Sudden increase in pain or swelling.
- Foul odor or pus-like discharge.
- Spreading redness or streaks around the wound.
- Fever or chills.
- Lack of any improvement after two weeks of care.
- Black or dead tissue around the wound edges.
- New numbness, weakness, or loss of function near the wound.
If you notice any of these red flags, seek urgent attention from a qualified wound care professional to prevent serious complications such as infections or tissue loss.
The Path to Healing With a Wound Care Doctor
Visiting a wound care doctor starts with a detailed evaluation to identify the wound type and underlying causes. This includes assessing your medical history, examining the wound’s appearance and measurements, and sometimes performing tests to gauge blood flow or detect infection. The specialist then creates a comprehensive treatment plan that may involve wound dressings, advanced therapies, lifestyle modifications, and coordination with other healthcare providers.
Regular follow-ups are crucial to monitor progress, adjust treatments, and ensure optimal healing conditions. Patient education on wound hygiene, nutrition, and risk factor management forms an important part of care as well.
Ready for Expert Wound Care?
If you or a loved one is dealing with a persistent wound, don’t delay in consulting a trusted wound care doctor. At Wells Surgical Services LLC, expert care is within reach to help identify your wound type, tailor your treatment, and promote effective healing.
Call today to schedule a consultation and take the first step toward recovery.